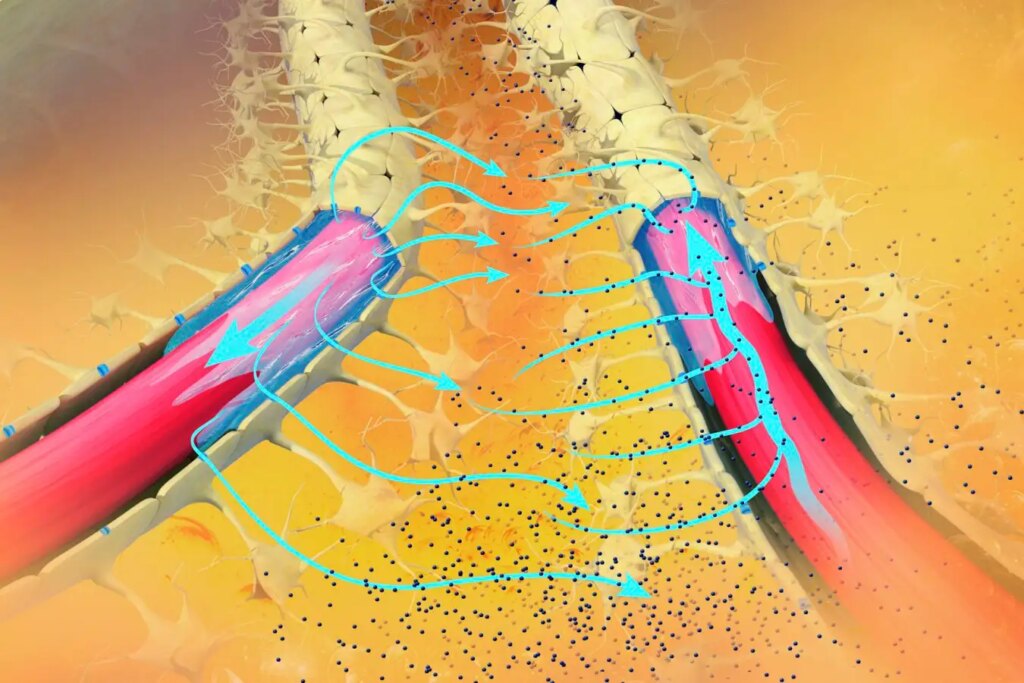
The glymphatic system facilitates the removal of brain waste products.
Klaus Renau/Science Photo Library
Researchers have discovered a groundbreaking drug that enhances the brain’s waste disposal system, effectively eliminating proteins linked to Alzheimer’s disease. A sedative commonly used in medical settings, when paired with a blood pressure stabilizer, shows promise in safely and efficiently clearing these toxic proteins, potentially delaying the disease’s onset by up to seven years.
“This is a significant advancement,” states Siju Gu from Harvard University, who was not part of the study. “While it may benefit individuals with neurodegenerative disorders, it could also enhance brain function in healthy individuals.”
The brain utilizes the glymphatic system, a vital network of channels surrounding blood vessels, to eliminate metabolic waste, directing it into the lymphatic system for blood disposal. This system is most active during deep sleep stages, wherein slow brain waves facilitate waste removal. However, its efficiency declines with age, especially in Alzheimer’s disease.
Previous research revealed that dexmedetomidine, a sedative widely used during procedures, boosts brain wave activity in mice. This enhancement improves the brain’s waste elimination capacity and slows cognitive decline in Alzheimer’s mouse models.
To assess dexmedetomidine’s effects in humans, Paul Dagham and his team at Applied Cognition, a pharmaceutical firm in California, enlisted 19 adults averaging 60 years of age. After a night of sleep deprivation in a controlled environment, blood samples were collected for baseline measurements.
Participants then received a four-hour infusion of dexmedetomidine alongside midodrine, a medication that mitigates low blood pressure, a common side effect of the sedative. Following a nap, additional blood samples were collected.
This experiment was replicated a few weeks later, with participants receiving a placebo and saline instead. The resulting analysis revealed that the combination of dexmedetomidine and midodrine, dubbed ACX-02, effectively removed amyloid and tau proteins—two proteins predisposed to misfolding and aggregation—better than the placebo treatment.
Dagham estimates that if ACX-02’s effects persist for several years, it could defer Alzheimer’s disease onset or progression by about seven years based on typical misfolded amyloid levels in those at risk. “This could significantly impact individuals at risk,” a research team member noted, including Jeff Iliff from the University of Washington.
Further analysis indicates that ACX-02 enhances the number of slow brain waves during sleep transitions and increases cerebral fluid flow, accelerating waste removal. Moreover, blood vessels appear to dilate and contract more effectively, enabling better fluid propulsion through the glymphatic system.
Though antibody therapies targeting amyloid plaques, such as lecanemab and donanemab, have received approval in the US and UK, their efficacy on symptoms remains minimal and they may cause hemorrhaging and swelling in the brain. “Innovative treatments are urgently needed. We know that the antibodies for Alzheimer’s are ineffective and can induce serious side effects,” asserts Natalie Beth Corner from the German Center for Neurodegenerative Diseases in Bonn.
No severe side effects were noted in Iliff’s trial. By enhancing the glymphatic system, there is less activation of the brain’s immune cells compared to antibody treatments, reducing risk factors associated with side effects, Dagham explains. ACX-02 additionally targets both amyloid beta and tau, which could augment its cognitive benefits. The research team plans to explore this further in patients with early Alzheimer’s disease.
Dr. Gu recognized that prior attempts to eliminate misfolded amyloid beta and tau in Alzheimer’s patients yielded limited success. However, he emphasized that if this novel approach proves safe and effective, it could see widespread application. “It may also benefit individuals with other neurodegenerative disorders linked to protein misfolding, such as Parkinson’s disease,” he states. Iliff adds that developing dexmedetomidine tablets could help treat diminished alertness due to sleep deprivation.
Topic:
Source: www.newscientist.com