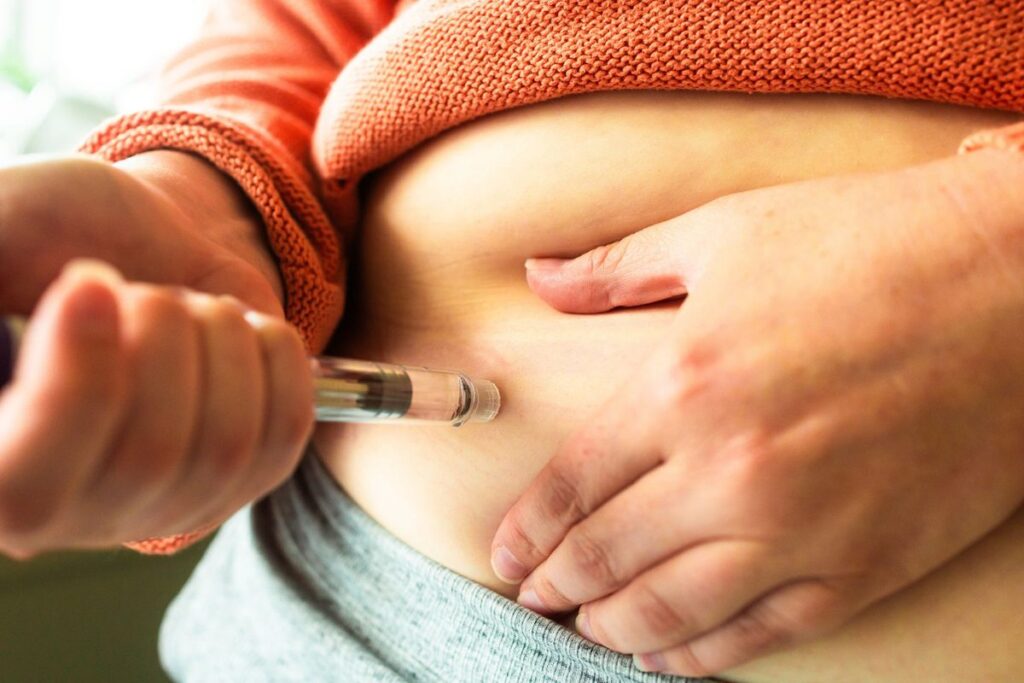
Weight loss doesn’t need to be an exhausting struggle anymore. Glucagon-like peptide-1 (GLP-1) medications, such as Ozempic, Wegovy, and Mounjaro, have transformed obesity treatment, offering remarkable results with just a simple injection.
Research indicates that adults taking the maximum doses can experience weight loss of over 20% of their body weight within 16 months, providing additional health benefits for the liver, heart, and brain.
This trend is gaining traction in the U.S., where nearly 12% of adults, or about 41 million people, have tried GLP-1 treatments. This phenomenon is also noted across the Atlantic, with an estimated 1.6 million adults in the UK using weight loss drugs last year.
While the rise of GLP-1 usage seems like a win for weight management, a hidden challenge may be emerging.
Recent studies reveal that many individuals begin to experience essential nutrient deficiencies shortly after starting these medications.
For instance, research from the Cleveland Clinic indicates that out of 460,000 adults prescribed GLP-1 drugs, nearly 20% developed a nutrient deficiency within a year, many without even realizing it.
Moreover, a separate study involving 480,000 GLP-1 users showed that 13.6% developed severe vitamin D deficiency within the first year, and approximately 60% didn’t get adequate iron or calcium from their diets.
The issue runs deeper. Another study suggests that GLP-1 drugs might deplete a range of vital nutrients, including magnesium, potassium, and vitamins A, C, D, and E.
“While these nutrients are required in small amounts, their importance cannot be overstated,” states Professor Giles Yeo, a specialist in neuroendocrinology and obesity at the University of Cambridge.
Additionally, adults on GLP-1 may also struggle to consume adequate protein and fiber.
Despite this prevalence, nutritional deficiencies often go unnoticed by healthcare providers, as many GLP-1 users are not monitored for their nutritional status. This oversight has been labeled a “major oversight” by professionals, as mentioned in a 2025 article in the International Journal of Obesity.
Dr. Stephen Heimsfield, director of the Metabolism and Body Composition Institute at Louisiana State University and lead author of the Cleveland Clinic study, emphasizes, “Obesity is a chronic disease that should be managed appropriately; this includes conducting nutritional blood tests if these medications are prescribed.”
read more:
Smaller Portions, Bigger Problems
So why are these deficiencies occurring? It largely relates to how these drugs alter food consumption.
GLP-1 medications mimic the natural satiety hormone, leading users to feel satisfied with smaller amounts of food, which is pivotal for weight loss.
However, this also reduces the chances of obtaining all necessary nutrients daily.
“Many people on these drugs may not have had a nutritious diet to start with, often lacking fresh produce and relying heavily on ultra-processed foods that lack essential nutrients,” explains Yeo.
“If you simply take medication without adopting better dietary habits, you’ll likely consume less food, which is not ideal,” he continues. “Neglecting to improve your diet can lead to nutritional deficiencies.”

Consequently, the deficiencies prevalent among GLP-1 users closely mirror those routinely observed in the general population. Common deficiencies include vitamin B12 and iodine among vegetarians and vegans, iron in menstruating women, and vitamin D in areas with limited sunlight exposure.
“These deficiencies are already fairly common,” Yeo adds, “and are likely to worsen with the use of GLP-1s.”
Moreover, these drugs not only limit dietary intake and heighten deficiency risk but may also lead to other side effects.
“GLP-1 treatment decreases food consumption but can also trigger gastrointestinal symptoms like vomiting and diarrhea,” notes Dr. Heimsfield.
“With diarrhea, there’s a risk of losing nutrients that haven’t yet been absorbed.” In effect, some nutrients may be expelled from the body before absorption can occur.
This problem is significant, with nearly one-third of GLP-1 users experiencing diarrhea; almost a quarter report nausea and vomiting.
Tip the Scales
Experts warn that the scale of this issue is concerning. With millions currently using GLP-1 drugs, a significant proportion of the population may be facing nutritional deficiencies without their knowledge.
“This is important,” asserts Heimsfield. “We should not assume GLP-1s are completely safe. Only time will reveal the long-term implications of these deficiencies.”
In severe cases, nutritional deficiencies can escalate into medical emergencies. Some individuals have been diagnosed with a severe neurological condition characterized by slurred speech and disorientation due to vitamin B deficiency linked to GLP-1 medications.

While such cases are rare, common vitamin D deficiency can have severe long-term health consequences for the broader population.
Dr. Heimsfield notes that low vitamin D levels may lead to bone loss (osteoporosis), increasing frailty risks in older adults. Additionally, insufficient protein intake can escalate the risk of losing muscle mass—a condition known as sarcopenia—with weight loss.
“Individuals who are obese at 70 and using these drugs could be inadvertently heading toward sarcopenia and frailty,” warns Heimsfield, increasing their chances of falls and fractures later in life.
A Tale of Two Diets
This growing issue is a “real concern,” Yeo states. “It’s crucial to recognize that many users of GLP-1s are well-off, often with less concern about their initial dietary habits.”
Indeed, most GLP-1 users in the UK acquire the drug privately, with monthly expenses often exceeding hundreds of dollars in the U.S. Consequently, these individuals are likely more affluent and capable of affording nutritious food.
Nevertheless, the emergence of new pill formulations of GLP-1 may eventually reduce costs and increase accessibility for a broader audience.
“At some point, a significant number of less fortunate individuals, many of whom are not in control of their food choices, may gain access to these drugs, which could pose serious challenges,” remarks Yeo.
While supplements can help mitigate specific micronutrient deficiencies, Yeo stresses that they are not a substitute for proper medical guidance for those on GLP-1.
“We’re not trying to alarm anyone, as these drugs are indeed powerful tools,” he concludes. “However, we must be vigilant regarding micronutrients, which are already common deficiencies that can worsen when diets are restricted.”
read more:
Source: www.sciencefocus.com