Misidentified ‘Cysts’ in PCOS are Not True Cysts
Steve Gschmeisner/Science Photo Library
Polycystic ovarian syndrome (PCOS) has undergone a significant rebranding. At the recent European Endocrine Society congress in Prague, renowned endocrinologist Helena Teed announced that it will now be referred to as polyendocrine metabolic ovary syndrome (PMOS).
This new terminology is more than just semantics; it corrects prevalent misconceptions about the condition. It highlights the crucial metabolic and hormonal features of PMOS that extend beyond the ovaries.
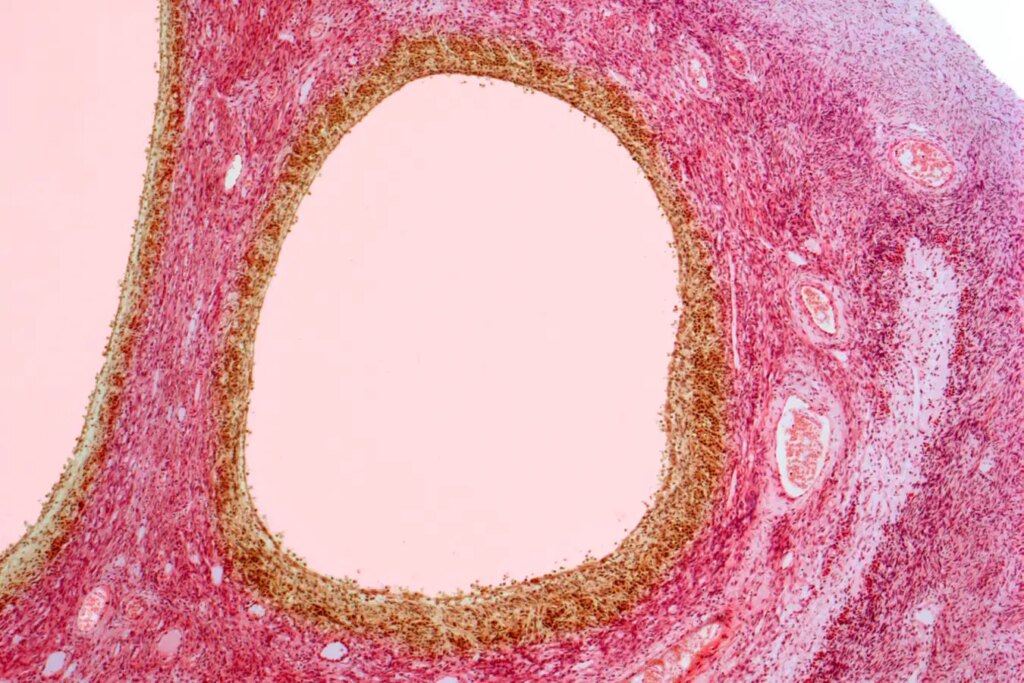
Reflecting on my diagnosis of PCOS over 20 years ago, I recall suffering from severe acne and irregular periods—common symptoms that prompted a distressing ultrasound. I was shocked to see what were labeled “cysts” on my ovaries. The fear of infertility and potential emergency surgeries left me feeling confused and devastated.
My journey led me to explore recent PCOS/PMOS research through New Scientist, unveiling the extensive misinformation surrounding the condition. After publishing an article on my findings in 2018, I discovered my story resonated with many others seeking clarity.
The major revelation is that the “cysts” associated with PCOS are misidentified; they are not cysts but rather underdeveloped eggs that remain trapped due to an excess of immature follicles in the ovaries. This shift in understanding allows for a more accurate perspective on ovarian health.
This overabundance can disrupt normal ovulation and menstrual cycles, potentially delaying pregnancy due to infrequent egg release. However, studies show that women with this condition are still likely to achieve their desired family size: 80% conceive without medication or IVF. Despite my challenges, including five miscarriages, I eventually had the three children I had always wanted.
Moreover, researchers now recognize that PMOS impacts the entire body, characterized by elevated male hormone levels like testosterone. This can lead to symptoms such as acne, excessive body hair, and thinning scalp hair. Insulin resistance is also prevalent, increasing the risk of weight gain, type 2 diabetes, hypertension, and cardiovascular issues. Mental health challenges, including anxiety and depression, are also common.
On a positive note, recent findings suggest that individuals with PMOS may have enhanced egg reserves, potentially delaying the onset of perimenopause and menopause, which could enhance reproductive options even in later years.
According to Tehi Piltonen, president of the International Society for Androgen Excess and Polycystic Ovary Syndrome and professor at Oulu University Hospital in Finland, the prevalence of this condition—affecting one in eight women—might have been advantageous for our ancestors, allowing them to store energy during times of food scarcity, thus prolonging pregnancy and reproductive viability.
While today’s environment of plentiful high-calorie foods presents challenges for those with PMOS, effective symptom management is available. Historically, attention was only given to ovarian health, particularly fertility concerns, but this new classification aims to broaden the approach.
Teed, who has campaigned for over a decade to reclassify PCOS, collaborated with 56 patient and professional organizations to establish a name that accurately reflects the science. If this change alleviates confusion and anxiety linked to former diagnoses, then the effort will have been well worth it.
Topics:
Source: www.newscientist.com